The menstrual cycle is closely connected to the autonomic nervous system, which helps regulate how your body responds to stress, rest, digestion, sleep, and emotional balance.⁸
Neurostimulation engages pathways involved in autonomic regulation. By stimulating external branches of the vagus and trigeminal nerves, it supports a shift away from elevated sympathetic activation and toward greater parasympathetic balance.²
This non-hormonal, non-pharmaceutical approach works with the nervous system to support the body’s natural regulatory processes during menstruation.
Shapes Your Cycle
Your Nervous System Shapes Your Cycle
Your Nervous System
The Sympathetic State
Prepares the body for action and heightened alertness. Heart rate increases. Breathing becomes faster or more shallow. Stress hormones rise, and digestion may slow or feel disrupted.
During menstruation, increased sympathetic activity can make these responses more noticeable, contributing to feelings of tension, discomfort, or imbalance.
The Parasympathetic State
Supports rest, recovery, and regulation. Heart rate slows. Breathing deepens. Digestion becomes more efficient. The body shifts toward repair and balance.
During menstruation, stronger parasympathetic activity supports steadier energy, emotional balance, and overall physiological stability.
Understanding Our Neural Pathways
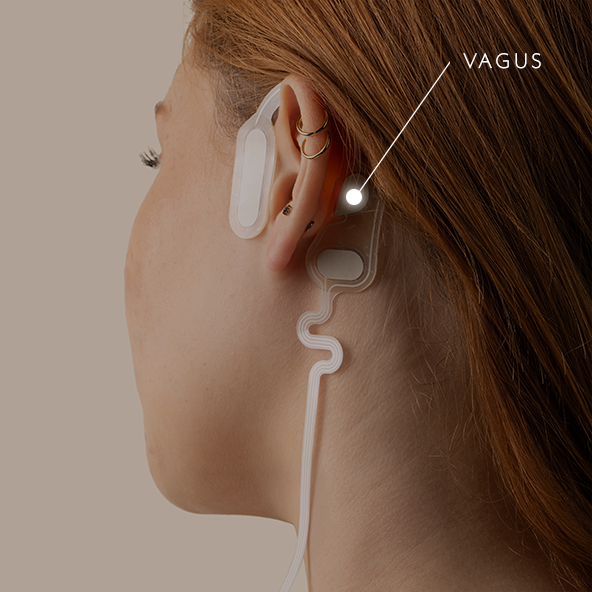
The Vagus Nerve
The Wandering NerveThe vagus nerve is one of twelve cranial nerves and the only one that extends beyond the head to connect with major organ systems throughout the body, including the heart, lungs, and spleen.
As a key part of the autonomic nervous system, it helps regulate digestion, sleep and energy, mood, and overall balance between stress and recovery. Because it connects to organs involved in blood-related processes, including the spleen, it is especially relevant in understanding menstrual health.¹ ⁶

The Trigeminal Nerve
The Sensory PathwayThe trigeminal nerve is one of the primary sensory nerves of the head and face. It plays a central role in how the brain interprets physical sensations, including signals related to comfort and discomfort.
Trigeminal pathways also connect to brain regions involved in neurochemical signaling, the brain’s internal messaging system. These pathways influence naturally occurring compounds such as endorphins (i.e. body’s natural pain killers) and other regulatory messengers, helping explain their relevance to comfort and overall well-being during the menstrual cycle.
Further Reading & References
- Ahmed, U., Chang, Y. C., Zafeiropoulos, S., Nassrallah, Z., Miller, L., & Zanos, S. (2022). Strategies for precision vagus neuromodulation. Bioelectronic medicine, 8(1), 9.
- Butt, M. F., Albusoda, A., Farmer, A. D., & Aziz, Q. (2020). The anatomical basis for transcutaneous auricular vagus nerve stimulation. Journal of anatomy, 236(4), 588-611.
- Czura, C. J., Weyand, A. C., Baldwin, M. K., Recht, M., McWade, M. A., Covalin, A., & Khodaparast, N. (2025). Transcutaneous auricular neurostimulation to reduce heavy menstrual bleeding in women with and without von Willebrand disease. Frontiers in Medicine, 12, 1664433.
- Mercante, B., Deriu, F., & Rangon, C. M. (2018). Auricular neuromodulation: the emerging concept beyond the stimulation of vagus and trigeminal nerves. Medicines, 5(1), 10.
- Kızkın, Z. Y., Yıldız, R., & Özden, A. V. (2025). Effects of Transcutaneous Auricular Vagus Nerve Stimulation in Individuals with Primary Dysmenorrhea: A Randomized Controlled Trial. Neuromodulation: Technology at the Neural Interface.
- Kim, A. Y., Marduy, A., de Melo, P. S., Gianlorenco, A. C., Kim, C. K., Choi, H., ... & Fregni, F. (2022). Safety of transcutaneous auricular vagus nerve stimulation (taVNS): a systematic review and meta-analysis. Scientific reports, 12(1), 22055.
- Percin, A., Ozden, A. V., Yenisehir, S., Pehlivanoglu, B. E., & Yılmaz, R. C. (2024). The effect of in-ear and behind-ear transcutaneous auricular vagus nerve stimulation on autonomic function: a randomized, single-blind, sham-controlled study. Journal of Clinical Medicine, 13(15), 4385.
- Roy, S., Agordati, E., & Wilcockson, T. D. (2025). Autonomic nervous system, cognition, and emotional valence during different phases of the menstrual cycle—a narrative review. NeuroSci, 6(3), 78.